It is possible that the long-elusive cause of Alzheimer’s disease has finally been discovered: Porphyromonas gingivalis, the key bacteria in chronic gum disease. If you bled when you brushed your teeth, you might want to get that checked out.
Gum disease affects roughly a third of the population. But the good news is that a drug that blocks the main toxins of P. gingivalis is entering major clinical trials this year, and research shows it might stop and even reverse Alzheimer’s.
Alzheimer’s is one of the biggest mysteries in medicine. There are many types and causes of dementia, but Alzheimer’s disease is the most common form, accounting for between 60 and 70%of all cases.
The condition, which results in progressive loss of cognitive function and memory, is disheartening for both the patients and their loved ones.
The disease often involves the accumulation of proteins called amyloid and tau in the brain. The leading hypothesis has been that the disease arises from defective control of these two proteins, especially amyloid, which accumulates to form large, sticky plaques in the brain.
In recent years, much research has revealed that people can have amyloid plaques without having dementia. So many efforts to treat Alzheimer’s by moderating these proteins have failed that the hypothesis has been seriously questioned.
Nevertheless, evidence has been growing that the function of amyloid proteins may be as a defense against bacteria. This has lead to a spate of recent studies looking at bacteria in Alzheimer’s, particularly those that cause gum disease, which is known to be a major risk factor for the condition.
Bacteria involved in gum disease and other illnesses have been found after death in the brains of Alzheimer’s patients, but until now, it hasn’t been clear whether these bacteria caused the disease or simply entered via brain damage caused by the condition.
New hypothesis from Cortexyme
Many scientific teams have been investigating P. gingivalis, and so far have found that it invades and inflames brain regions affected by Alzheimer’s; that gum infections can worsen symptoms in mice genetically engineered to have Alzheimer’s; and that it can cause Alzheimer’s-like brain inflammation, neural damage, and amyloid plaques in healthy mice.
Stephen Dominy of Cortexyme, a pharmaceutical firm in San Francisco, and his colleagues are studying toxic enzymes called gingipains that P. gingivalis uses to feed on human tissue. In their study, they found gingipains in 96%of 54 Alzheimer’s brain samples taken from the hippocampus – a brain area important for memory. Upon examining the DNA of three Alzheimer’s brains, the bacteria itself was found as well.
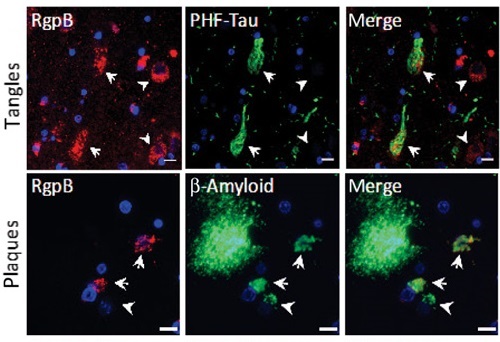
P. gingivalis is an asaccharolytic Gram-negative anaerobic bacterium that produces major virulence factors known as gingipains, which are cysteine proteases consisting of lysine-gingipain (Kgp), arginine-gingipain A (RgpA), and arginine-gingipain B (RgpB).
This work is the first report showing P. gingivalis DNA in human brains, and the associated gingipains, co-lococalising with plaques. This study is also the first to show that gingipains slice up tau protein in ways that could allow it to kill neurons, causing dementia. RgpB was associated with paired helical filament Tau (PHF-Tau). Intracellular Amyloid-β was often colocalized with RgpB.
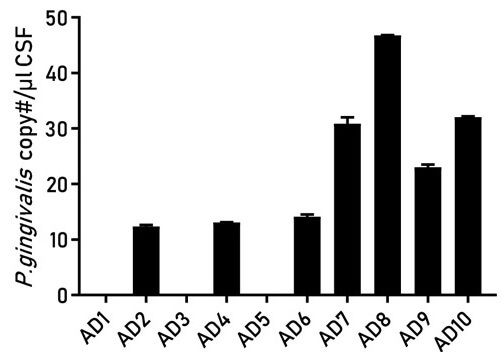
Porphyromonas gingivalis and its enzymes were found at higher levels in those who had experienced worse cognitive decline, and had more amyloid and tau accumulations. Researchers also found this bacteria in the spinal fluid of living Alzheimer’s disease patients, which suggests that this technique may provide a method of diagnosing the disease.
Researchers of Cortexyme had previously developed gingipain blockers. In mouse studies, these blockers decreased brain inflammation and stopped the production of beta amyloid.
Cortexyme also reported that their gingipain blockers have undergone initial human safety tests, and appear to improve the condition of patients with Alzheimer's disease. The firm also plans to launch a larger trial of the drug.
Additionally, Cortexyme plans to test gingipain blockers against gum disease itself. Efforts to fight periodontal disease have led a team in Melbourne to develop a vaccine for P. gingivalis that started tests in 2018. A vaccine for gum disease would be welcome – but if it also stops Alzheimer’s the impact could be enormous.
