
Procalcitonin is a biochemical marker that holds great promise for the management of infectious diseases, particularly infections of the respiratory tract and sepsis.
Besides respiratory infections and other infectious diseases, multiple recent studies have investigated the possible benefits of PCT testing in patients with cardiovascular disorders, including shortness of breath and possible heart failure, suspected endocarditis, cardiac arrest, and acute coronary syndromes, among others. In patients with shortness of breath, observational studies as well as a secondary analysis of a randomized trial found initial PCT levels to have high prognostic value. These investigators reported worse clinical outcomes in patients treated with antibiotics over diuretics and nitrates despite their having low PCT levels that strongly suggested the absence of bacterial infection.
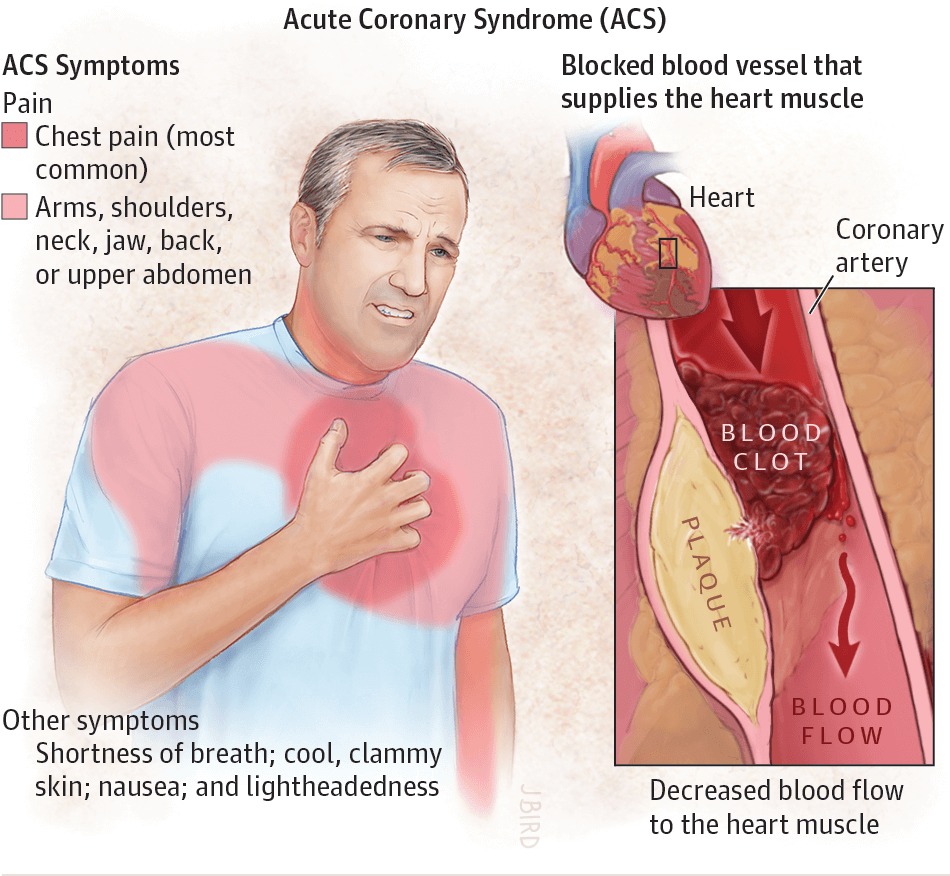
Interestingly, there is growing evidence linking PCT to the extent of atherosclerosis and prognosis in patients with coronary artery disease. It is well known that inflammation plays a role in the pathophysiology of atherosclerosis. Additional inflammatory markers are also known to be elevated in patients with acute myocardial infarction, with CRP having been shown to predict the risk of recurrent events. Levels of PCT have been shown in multiple studies to be elevated in patients with acute coronary syndromes, particularly in complicated cases.
Infective endocarditis is a life-threatening disease caused by infection of the endocardial surface of the heart, usually involving the heart valves, mural endocardium, or a septal defect. Infective endocarditis continues to pose a diagnostic challenge for clinicians because of the various clinical presentations. This is mirrored in the current definition (i.e., modified Duke's criteria) that integrates clinical findings, microbiological study results, and imaging findings. These criteria over- and under-diagnose infective endocarditis, particularly in patients with subacute disease and atypical presentations. In light of the expected benefits of early antibiotic treatment in patients with infective endocarditis, a sensitive marker for this condition would be highly desirable and may potentially improve outcomes. Importantly, multiple studies have observed PCT to be highly associated with bacteremia-the main diagnostic criteria for endocarditis-in Emergency Department patients with fever.
In patients with coronary heart disease and atherosclerosis, PCT has shown prognostic value and its levels correlate with adverse clinical outcomes and severity status. Large-scale studies looking at the additive value of PCT when used with established markers are currently lacking. Knowledge of the utility of PCT may become increasingly important for the cardiologist working in the emergency care setting. If the interventional studies suggested above show positive results, PCT may evolve into an important additional biomarker with the potential to significantly improve the management of polymorbid patients with cardiovascular disease.
